Introduction
Food-borne outbreaks cause wide range of illnesses from bacterial, viral, protozoal and chemical contamination of food.1 Most deaths in hospital are due to bacterial agents, however viruses cause half of the food bore diseases.2 Pathogens cause a large spectrum of these infections or intoxications, such as enteric complications, abdominal pain, fever, hemorrhagic colitis, bloodstream infection, meningitis, joint infection, kidney failure, paralysis, miscarriage, etc that was reported previously.3 The common manifestation of food poisoning occurs by diarrheal diseases, which is often caused by a toxin released from microbes.4, 5 WHO estimates that globally food-borne and waterborne diseases together kill about 2.2 million people annually, 1.9 million of whom are children.4, 6 In Bangladesh, diarrhoea is responsible for one-third of childhood deaths, the actual number of casualty might be underestimated in the absence of a national health database. The insufficient data on food-borne infection shows 501 diarrhoeal cases are reported daily during monsoon seasons.6, 7, 8 Due to the absence of regular monitoring, assessment of the public health impact of food-borne illnesses is a tedious task. Ready-to-eat foods are often consumed at the sale points in the ready food conditions and it could be cooked or raw, hot or chilled consumed without any types of further cook treatment.9, 10 Traditional food habits of general Bangladeshi people are changing with passing time due to rapidly modified and urbanization. Changing lifestyle, the involvement of the woman in official jobs and change in the family structure are encouraging more people to consume ready-to-eat food in contrast to the home-cooked food which was the common practice in the last century. In the current economical edge, many local food factories process traditional food items and market them in small packs, commonly known as ‘home-made’ items. Unfortunately, such food items are sold by groceries, departmental store, vendors and super shops without the supervision of authorities. These ready-to-eat foods often substitute homemade foods and are important for the nutritional status of the urban population. The unhygienic condition during production, preparation and selling of food often deteriorates the microbiological quality of food items.11 At present, the tendency of consuming ready-to-eat food products has increased tremendously. Attractive packages, marketing on a reputed shop and good advertisement strategies encourage people to consume certain products without checking for food safety and nutritional information. Generally, the food manufacturers in Bangladesh need to obtain a license from Bangladesh Standard Testing Institute (BSTI) to market their products. BSTI follows the guidelines of the International Organization for Standardization (ISO) to ensure food safety.12, 13 High-risk pathogens like Campylobacter spp., verotoxigenic Escherichia coli (VTEC), Salmonella spp., Shigella sp. and V. cholera should is absent in ready-made foods according to food quality standards.14
This microbiological study showed the prevalence of considerable numbers of aerobic and coliform bacteria in ready-to-eat food. This study also pointed out that multidrug-resistant bacteria might be dispersing over the population through contaminated ready-to-eat foods, an observation shared by similar reports from independent groups.1 To assess the potential risk to public health this study also suggested conducting a detailed microbial analysis and profiling their drug-resistance patterns. Consequently, the purpose of this study was to appraise the microbial status of food-borne pathogens, spoilage bacterial content, and food processing hygiene different ready-to-eat foods from Dhaka city, Bangladesh.
Materials and Methods
Sample Collection and Enrichment Procedure
Microbiological analysis of the ready-to-eat food samples was collected at random from the local shops and vendors in Banani area in Dhaka city. Sampling sites comprised of the most crowded places. 18 categories of food items were purchased in triplicates from local street vendors and local superstore of Banani, Dhaka city from August 2016 to February 2017. Collected samples were taken to the (Centre of Excellence) Laboratory, Department of Microbiology of Primeasia University, Dhaka, within the earliest time from purchase for further processing and analysis.12 Solid food samples were collected in pre-sterilized Stomacher bags (165mm x 150mm x 0.55mm). Fresh juice samples were collected in sterile Duran Bottles and transported in the icebox. All samples were analyzed according to the standard microbiological methods for food analysis.15
Microbiological Analysis
For determining the microbial load in samples, the total viable count (TVC) and total coliform count (TCC) were determined with the spread-plate method. The plate count agar and MacConkey agar (Oxoid Ltd, Hampshire, UK) respectively used to indicate the TCC and TVC for the collecting samples.1gof each sample was diluted in 10-folds in sterile normal saline water (0.85% NaCl) and properly diluted up 10-1 to 10-6 decimal in normal saline water.12 100µL from each dilution of each sample were spread on selected media by spread plate method with sterile glass spreader. Plates were incubated overnight at 37°C and visible colonies were counted and represented as CFU/g or CFU/mL in log scale. Cell counts (CFU/g and CFU/mL) were derived from the average of 3 independent experiments (Fig. 1).16, 17, 18
Isolation and Identification of Microorganism
Twenty-five grams (25g) of each sample was homogenized in 225 millilitres of buffered peptone water (Oxoid Ltd, Hampshire, England) and incubated overnight at 37°C. One millilitre pre-enrichment culture was mixed with 10 millilitres of Henja-Tetrathionate Broth (HiMedia Laboratories, Mumbai, India) and was incubated at 37ºC for 24 hours.1 The culture broths were subsequently streaked onto Salmonella-Shigella Agar (SS) media (Oxoid Ltd, Hampshire, England) and Bismuth-Sulphite Agar (BSA) media (HiMedia Laboratories, Mumbai, India). Presumptive identification of each colony came from biochemical tests and biochemically confirmed isolates were re-confirmed with API 20E kits (BioMerieux, Inc.).12, 19
Twenty-five (25g) of each sample was homogenized in 225 millilitres of buffered peptone water (Oxoid Ltd, Hampshire, England) and pre-enriched by incubating for overnight at 37°C. One millilitre of pre-enrichment culture was mixed with 9-millilitre lactose broth medium (Oxoid Ltd, Hampshire, England) with Durham fermentation tubes and incubated overnight at 37°C. After incubation periods, the faecal coliform microorganisms produce gas in the Durham tube.18 Then one loop-full culture broth was streaked onto Eosine-Methylene Blue Agar (EMB) (Oxoid Ltd, Hampshire, England) incubated for 24 hours at 37°C to identify E. coli. The identification of the isolates to genera was confirmed with API20 (BioMerieux, Inc.) (Table 1). The E. coli isolates were tested for detection of β-glucuronidase on Escherichia coli-methyl umbiliferylglucuronate (EC-MUG, Oxoid, New Hampshire, England) medium under standard bacteriological conditions (Table 2).
Biochemical tests for Identification of Isolates
Pure colonies from nutrient agar (NA) plates were taken for biochemical tests such as Kligler Iron Agar (KIA) (HiMedia Laboratories, Mumbai, India), Simmons citrate agar media, MR-VP media for Methyl red and Voges-Proskauer test, SIM media for Indole and motility test (Oxoid Ltd, Hampshire, England), Oxidase and catalase test for super-oxide dismutase and hydrogen peroxide20 and API 20E kits (BioMerieux, Inc.) for biochemical profiling.20
Antibiogram (Antibiotic Susceptibility Profile) Test
Susceptibility of isolated strains was tested in vitro towards different antimicrobial agents through the Kirby-Bauer method using antibiotic disc diffusion on Muller-Hinton agar.21 It allowed determination of the action of the antibiotic which shows the inhibition of the pathogen to the degree proportional to the diameter of the zone of inhibition that resulted from diffusion of the antimicrobial that surrounding the disc onto the agar medium. Commercial antibiotic discs were used in this experiment; Ampicillin 10µg (AMP), Azithromycin 15µg (AZM), Ciprofloxacin 5µg (CIP), Gentamicin10µg (CN), Kanamycin 30µg (k), Sulfamethoxazole 25µg (SXT), Tetracycline 30µg (TE). Briefly, 5 mL of Mueller–Hinton broth was inoculated with a pure culture of a specific isolate and incubated overnight at 37 °C. The 0.5 McFarland standard was used to adjust to the turbidity of actively-growing broth cultures.22 The intensity of antibiotic action was interpreted from the National Committee for Clinical and Laboratory Standards.22, 23, 24
Result
In this study, different kinds of “Ready-to-eat” food including sugarcane juice, lemon juice, kata pitha, chetoipitha (traditional rice cookies), carrot halwa, Nakshipitha (sweetened dissert), nan (bread), potato chips, singara, egg chop, potato chop, spring roll, chicken meatball, chicken samosa (fried snacks), burger, jhalmuri (Spicy puffed rice), borhani (spiced yogurt drink), hog plum chutney (pickle) were analyzed. The total viable count and total coliform count from these foods are given in Fig.1. Some specific food like a spring roll, sugarcane had both spoilage flora and bacterial pathogens as stated by others before.25, 26, 27
The API-20 test was done on selected isolates of. coli, Enterobactersakazaki, Citrobacterfreundii and Salmonella Typhimurium conform the result of the biochemical test (Table 2). The E. coli isolates were further cultured on EC-MUG medium (Oxoid, Hampshire, England) to observe the presence of β-glucuronidase with the probability of finding E. coli O157: H7, because the dangerous E. coli O157: H7 strains are negative for β-glucuronidase (Table 3).28,29 Finally, the antibiotic resistance pattern of the isolates indicated Ampicillin and Sulfamethoxazole resistance (Figure 2 and 3).
The Rifampicin was used as the negative control for antibiotic susceptibility test.
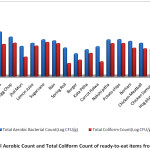 |
Figure 1: Total Aerobic Count and Total Coliform Count of ready-to-eat items from Dhaka city Click here to View figure |
Table 1: Biochemical profile of bacterial isolates from ready-to-eat foods from Banani
| Isolated strains | KIA | H2S | Indole test | MR test | VP test | Citrate test | Oxidase test | Catalase test | Motility | Gram stain | ||
| Slant | Butt | Gas | ||||||||||
| E. coli | Y | Y | + | – | + | + | – | – | – | + | + | Rod, (-) |
| Salmonella sp. | R | R | – | + | – | + | – | – | – | + | + | Rod, (-) |
Note: KIA= Kligler’s Iron Agar, Y=Yellow (Acid), R=Red (Alkaline), MR=Methyl red, VP=Voges-Proskauer test, positive= (+), Negative= (-)
Table 2. API-20 identification tests for bacterial isolates from the ready-to-eat food samples from Dhaka, Bangladesh
| y | Percentage of API in an isolated microorganism |
| Singara | E.coli-97.7% |
| Egg Chop | E.coli-99.7% |
| Lemon Juice | E.coli-99.7% |
| Sugarcane | E.coli-98% |
| Nan | Entrobactersakazaki- 98% |
| Kata Pitha | E.coli-99.9% |
| Potato chips | E.coli-95.8% |
| Nakshipitha | E.coli-99.7% |
| Chicken Samosa | Citrobacter freundii-99.7% |
| Hog plum chutney | E.coli-99.5% |
| Lemon Juice | Citrobacter freundii-96.9% |
| Singara | Salmonella typhimurium -97.5% |
| Egg Chop | Salmonella typhimurium -95.5% |
| Sugarcane | Citrobacter freundii-99.9% |
Table 3: Production of β-glucuronidase from the E. coli isolates from ready-to-eat food items from Dhaka
| Sample name | β-glucuronidase |
| Singara | + |
| Egg Chop | + |
| Lemon Juice | + |
| Sugarcane | + |
| Kata Pitha | + |
| Nakshipitha | + |
| Potato chips | + |
| Hog plum chutney | + |
Note: positive= (+), Negative= (-)
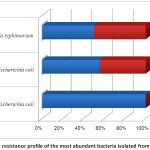 |
Figure 2: Antibiotic resistance profile of the most abundant bacteria isolated from ready-to-eat food Click here to View figure |
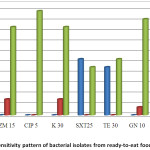 |
Figure 3: Antibiotic sensitivity pattern of bacterial isolates from ready-to-eat food samples from Dhaka Click here to View figure |
Note: Name of antibiotics disc: AMP=Ampicillin, AZM=Azithromycin, CIP=Ciprofloxacin, K=Kanamycin, SXT = Sulfamethoxazole, TE =Tetracycline, GN=Gentamicin
Discussion
In Bangladesh, food contamination exposes consumers to food-borne hazards. Lack of awareness and lack of adherence to the food laws and regulation together within the frequent implementation of existing regulations are contributing significantly to dissatisfactory food safety circumstances of Bangladesh.2, 6 Street-vended, ready-to-eat food items are becoming a globally growing trend for ease, quickness and convenience.30,31 As per a report, a range of food-borne infections are the cause of most microbial diseases. In developing countries, a high level of mortality rate is found due to bacterial diarrhoea.32 The frequency of typhoid among the city slum-dwellers is estimated at 3.9 episodes per year when screening in one thousand people. whereas in case of pre-school children who are aged between 2 to 5 years were estimated to be 8.9 times more at a risk of getting infected by typhoid.29 Among the diarrhea affected people in Dhaka city, Salmonella covered 6.4% of the bacterial isolates.32 Contaminated water, food and person-to-person contact are the important sources of Salmonella spp. and E. coli.This study emphasizes the role of sub-standard food items retailed in the super-shops as a source of Salmonella spp. and E. coli infection. Globalization has made foreign items like chicken nuggets and sausages popular to the urban youth. Moreover, the popular traditional items like rice cookies (pitha), mashed sweets (Halwa) and hard caramels (Badampapri, Helen papri) are only marketed by small-scale industries popularly advertised as ‘Homemade’ products. The name, number and location of these traditional small-scale producers (Home-made brand) are not recorded with the Bangladesh Standard Testing Institute (BSTI). The BSTI approval does not appear on the packages of the homemade brands. The occurrence of high Total Heterotrophic Count (HTC) and relatively high Total Coliform Count (TCC) reflect the poor quality of the finished product (Fig. 1). Fried foods like potato chops, egg chop, singara, chicken meat ball, baked items like Nan, sugary foods like sugarcane juice, nakshipitha have a high burden of TAC (6x 106 CFU/mL) ) and TCC (>4x 106 CFU/mL) (Fig 1). E. coli was found as the dominant species from singara, egg chop, lemon juice, sugarcane juice, kata pitha, potato chips, nakshipitha and hog plum chutney (Table 2). All isolates of E. coli were β-glucuronidase positive (Table 3). Enterobactersakazaki was found in Nan bread. Citrobacterfreundii was isolated from chicken samosa, lemon juice and sugarcane juice. Potential pathogen Salmonella typhimurium was isolated from singara and egg chop. The other important aspect of the identification of food pathogens is to assess the burden of multi-drug resistant pathogens. Simultaneous resistance against Ampicillin and Sulfamethoxazole makes it difficult to treat an infection. Successive spread in resistance poses a hazard of an epidemic by resistant E. coli with a little therapeutic option. This could be particularly grim in Bangladesh since the infectivity of common, affordable and well-tolerated drugs might mean a hike in mortality. On the contrary to the published reports the E. coli isolates were susceptible to the common antibiotics (Fig 3), indicating a reduced risk of therapeutic failure. E. coli isolates were resistant against Ampicillin, Sulfamethoxazole and Tetracycline. The occurrence of β-glucuronidase positive strains means lesser risks because of the very-toxigenic. coli are often β-glucuronidase negative. The circumstance is more threatening in young children and the population. Presence of E. coli in processed and packaged food indicated poor handling and lack of adherence to good manufacturing practice by the local manufacturers.33, 34, 35 Awareness among food producers, consumers, retailers and the inspection authority might improve the situation of food safety in Dhaka city.
Conclusion
The current study exhibited that, the microbiological quality of the ready-to-eat street foods available in Dhaka city, Bangladesh, expose the customers to the high risk of acquiring food-borne diseases from multi-drug resistant bacterial pathogens.
Competing Interests
Authors have declared that no competing interests exist.
Acknowledgement
This project has been supported by grants from Primeasia University Center of Excellence.
Reference
- Khare S., Tonk A., Rawat A. Foodborne diseases outbreak in India: A Review. Int J Food Sci Nutrition. 2018; 3(3): 9-10
- Noor R, and Feroz FN. Microbiological Quality of Commonly Consumed street foods in Bangladesh. Nutrition and Food Science. 2016. 6(1):1-6
CrossRef - Sultana S., Tarafder G.H., Siddiqui T.A., Sharma B.C., Walliullah M., Ahmed T., Munna M.S., Noor A.F., PopyK., Das K.K., Acharjee M., Urmi N.J., Rahman T. and Noor R. Microbiological quality analysis of shrimps collected from the local market around Dhaka city. International Food Research Journal. 2014; 21(1): 33-38
- Fernandez-Segovia I., Perez-Llacer A., Peidro, Fuentes A. Implementation of Food Safety Management Systems according to ISO 22000 in the Food Supplement Industry: A Case Study. 2014. 43:28-34
- Teplitski M., Wright A.C. and Lorca G. Biological approach for controlling shellfish-associated pathogens. Current Opinion in Biotechnology. 2009; 20:185–190.
CrossRef - World Health Organization Bangladesh (WHO Bangladesh). January 2018. Areas of work: Food Safety. Retrieved on March 2, 2018, from WHO Bangladesh Website: http://www.searo.who.int/bangladesh/areas/foodsafety/en/
- Nyenje ME., Odjadjare CE., Tanih NF., Green E., Ndip RN. Foodborne Pathogens Recovered from Ready-to-Eat Foods from Roadside Cafeterias and Retail Outlets in Alice, Eastern Cape Province, South Africa: Public Health Implications. Int J Environ Res Public Health. 2012; 9(8): 2608–2619.
CrossRef - Country Paper on Audit on the implementation of environmental policy & Role of Supreme Audit Institutions in promoting national sustainable development. Retrieved on November 20, 2018, from the official website available: http://www.audit.gov.cn/en/n1066/n1067/n1071/n1072/c89202/attr/345669.pdf
- Kinman LA., Garcia MBM., Speshock J., Harp RM. Presence of pathogenic bacteria in ground beef during consumer thawing and food-handling habits. J Food Microbiol. 2018; 2(2): 12-14
- Tsang D. Microbiological guidelines for ready to eat food Road and Environmental Hygiene Department Hong Kong. Report of the Food and Environmental Hygiene Department, Hong Kong. 2002; pp: 115-116.
- Nguendo Yongsi HB. Eating to Live or Eating to Damage One’s Health: Microbiological Risks Associated with Street-Vended Foods in a Subtropical Urban Setting (Yaoundé-Cameroon). Nutri Food SciInt J. 2018; 6(4): 555695.
- Banik A., Mohammad N., Akter T., Fatema K., Abony M. ‘Prevalence, Identification and Antibiotic Susceptibility of Enterococcus species Isolated from Chicken and Pigeon meat in Gazipur Area, Bangladesh. Open J Med Microbiol. 2018. 8(3):307-10
CrossRef - Bangladesh Standard and Testing Institute (BSTI). Retrieved on March 2,2018from BSTI Bangladesh Website available: bsti.gov.bd
- Public Health England-GOV.UK. November 2009. Publications: Guidelines for Assessing the Microbiological Safety of Ready-to-Eat Foods Placed on the Market. Retrieved on March 10, 2018, from Public Health England website: http://www.hpa.org.uk/webc/hpawebfile/hpaweb_c/1259151921557
- European Commission. November 2006. Guidance document on official controls, under Regulation (EC) No 882/2004, concerning microbiological sampling and testing of foodstuffs. Retrieved on March 13, 2018, from the European Commission website: http://ec.europa.eu/food/food/controls/foodfeed/sampling_testing.pdf
- Misra S., Raghuwanshi S., Gupta P., Saxena RK. Examining growth inhibitor pattern and lactic acid production in Streptococcus mutans using different concentrations of xylitol produced from Candida tropicalis by fermentation. Anaerobe. 2012;18(3):273-9.
CrossRef - Malek M., Akter J., Ahmed T., Uddin MU. Isolation and quantification of microorganisms from some common milk products within Dhaka city, Bangladesh. Stamford J Microbiol. 2016; 5(1), 13-17
CrossRef - Rabbi FA., Rabbi F., Runun, Zaman K., Rahman M., & Noor R. Microbiological Quality Assessment of Foods collected from Different Hospitals within Dhaka City. Stamford Journal of Microbiology,1(1): 31-36.
- Gowrishankar S., Poornima B., Pandian SK. Inhibitory efficacy of cyclo (L-leucyl-L-prolyl) from mangrove rhizosphere bacterium-Bacillus amyloliquefaciens (MMS-50) toward cariogenic properties of Streptococcus mutans. Res Microbiol. 2014; 165(4):278-89.
CrossRef - Bergey DH and Holt JG. Bergey’s Manual of Determinative Bacteriology (ed. 9). 2000. Lippincott-Williams Inc.
- Bauer AW., Kirby WM., Sherris JC and Turck M. Antibiotic susceptibility testing by a standardized single disk method. American journal of Clinical Pathology. 1966; 45(4): 493–496.
CrossRef - Biswajit Modak, Md. Shahinur Rahman, Mohammad Shahid Gazi, Md. Aftab Uddin and Tasmina Rahman. Antimicrobial potency assay of common antibiotics collected from different drug stores in Dhaka Metropolis. Stamford J Microbiol. 2013; 3(1): 26-29
CrossRef - National Committee for Clinical Laboratory Standards (2007). Reference method for broth dilution antifungal susceptibility testing of yeasts; approved standard. https://wwwn.cdc.gov/cliac/pdf/addenda/cliac0904/addendum_w.pdf
- McConnel CS., Shum L, House JK. Antimicrobial susceptibility of Australian bovine Moraxella Aust Vet J. 2007. 85(1-2):70-71.
CrossRef - Akinnibosun FI, Ojo KN. Comparative study of ready-to-eat foods from road-side and eateries in Benin City, Nigeria. 2015. 9(13):929-933
- Chowdhury FFK, Acharjee M, Noor R. Maintenance of Environmental Sustainability Through Microbiological Study of Pharmaceutical Solid Wastes. Clean – Soil Air Water 44(3)
CrossRef - Shammi T. Detection of Vibrio spp., Salmonella spp., and Shigella spp. among the frozen food samples employing the enrichment culture technique. Stamford J Microbiol. 2015. 5(1):26-29
CrossRef - Ahmed T, Baidya S, Acharjee M, Rahman T. Qualitative analysis of drinking water through the most probable number (MPN) method. Stamford J Microbiol. 2013. 3(1): 9-16
CrossRef - Ahmed, D., Hoque, A., Elahi, MS., Endtz, HP., and Hossain, MA. Bacterial aetiology of diarrheal diseases and antimicrobial resistance in Dhaka, Bangladesh, 2005-2008. Epidemiol Infect. 2012; 140(9):1678-84.
CrossRef - Sarker, N., Islam, S., Hasan, M., Kabir, F., Uddin, M.A. and Noor, R. Use of multiplex PCR assay for detection of diarrheagenic Escherichia coli in street vended food items. American Journal of Life Sciences. 2013; 1(1): 267-272.
CrossRef - Ahmed, M. S. U., Nasreen, T., Feroza, B. and Parveen, S. Microbiological quality of local market vendor freshly squeezed fruit juices in Dhaka city, Bangladesh. Bangladesh Journal of Scientific and Industrial Research. 2009; 44(4):421-424.
CrossRef - Das SK, Ahmed S, Ferdous F, Farzana F.D, Chisti M.J, Latham J.R, Talukder K.A, Rahman M, Begum Y.A, Qadri F, Faruque A.S.G and Ahmed T. Etiological diversity of diarrhoeal disease in Bangladesh.J Infect DevCtries. 2013; 7(12):900-9.
CrossRef - Sousa CPd. The impact of food manufacturing practices on foodborne Braz. arch. Biol. Technol. 2008; 51(4):58-64
- Malavi ND, Muzhingi T and Abong GO. Good Manufacturing Practices and Microbial Contamination Sources in Orange Fleshed Sweet Potato Puree Processing Plant in Kenya. Int J Food Sci. 2018; 2018: 4093161.
- Prevention of VTEC Infection: Report of the Scientific Committee of the Food Safety Authority of Ireland 2010. file:///C:/Users/Tasnm/Downloads/E.%20coli%20report%202010%20FINAL.pdf

This work is licensed under a Creative Commons Attribution 4.0 International License.






